 
The much more common microvesicular variant of hyperplastic polyp has been referred to as mucosal hyperplasia and metaplastic polyp in the older literature however, those terms are no longer recommended. Rather, it is important to recognize the subtler features of the goblet cell variant of hyperplastic polyp (goblet cell hyperplastic polyp) in order to distinguish this from normal mucosa and to separate it from other types of serrated polyps. Two types of hyperplastic polyp are recognized morphologically however, it is not yet necessary to distinguish between these two variants in clinical practice. Table 1 provides a classification scheme of serrated colorectal polyps along with key morphologic and molecular features. Finally, an update on serrated polyposis, as well as colorectal carcinomas arising from serrated precursors will be provided. The emerging data on the natural history of serrated precursors will be emphasized in addition to the features that should guide future colonoscopy surveillance intervals. 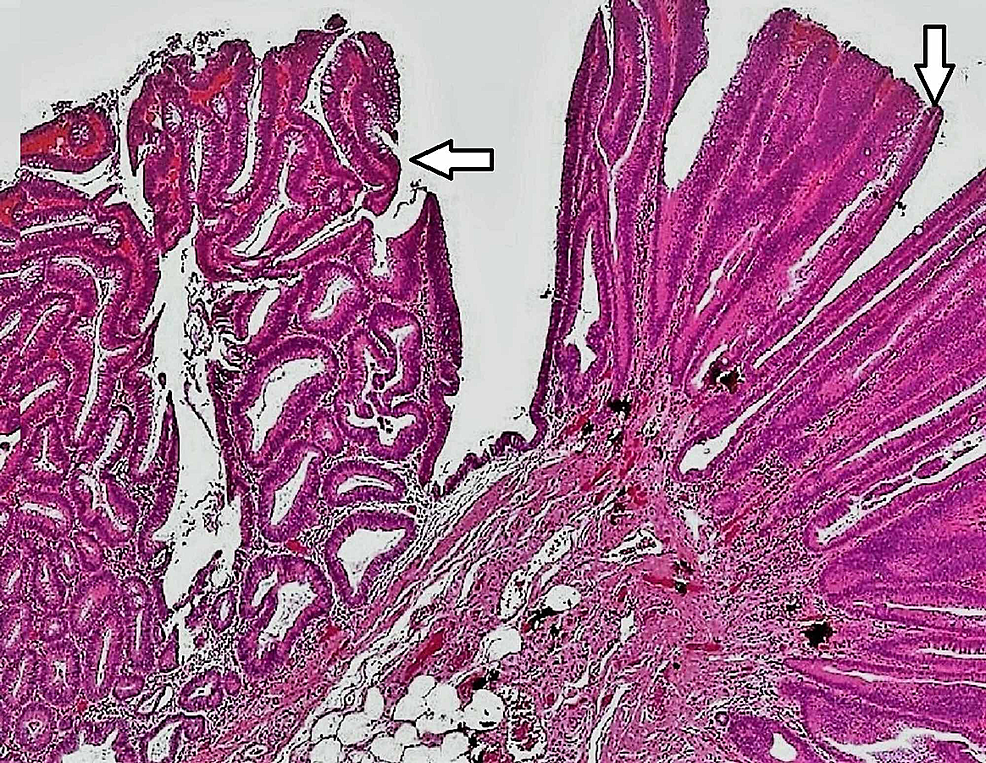
Key morphologic features that are necessary for proper classification will be presented and unusual serrated lesions that do not fit neatly into a specific category will be discussed. This review will summarize the classification and molecular characterization of serrated polyps. These polyps are also molecularly heterogenous and can give rise to carcinomas with divergent clinical outcomes. Serrated polyps range in morphology from polyps with only superficial serrations to those with exaggerated serrated architecture and overt dysplasia. It is now recognized that up to at least 20% of colorectal carcinomas arise not through conventional adenomas but rather through serrated polyps. While the conventional adenoma has long been recognized as a precursor to colorectal carcinoma and served as the primary driver of post-polypectomy surveillance guidelines, work over the past few decades has identified and characterized other precursor lesions. Colonoscopy also allows for identification of patients at higher risk for developing metachronous lesions based on pathologic review of polypectomy specimens. Both colonoscopic surveillance and/or stool-based tests are utilized in most counties but only colonoscopy allows for resection of precursor lesions. Your health care provider might recommend stopping proton pump inhibitors or removing the polyp or both.Detection and removal of premalignant lesions is the guiding principle of colorectal carcinoma screening programs. These polyps are generally small and aren't a cause for concern.Ī fundic gland polyp with a diameter larger than about 2/5 inch (1 centimeter) carries a small risk of cancer. Fundic gland polyps are common among people who regularly take proton pump inhibitors to reduce stomach acid. Regular use of certain stomach medications. Familial adenomatous polyposis also can cause adenomas. 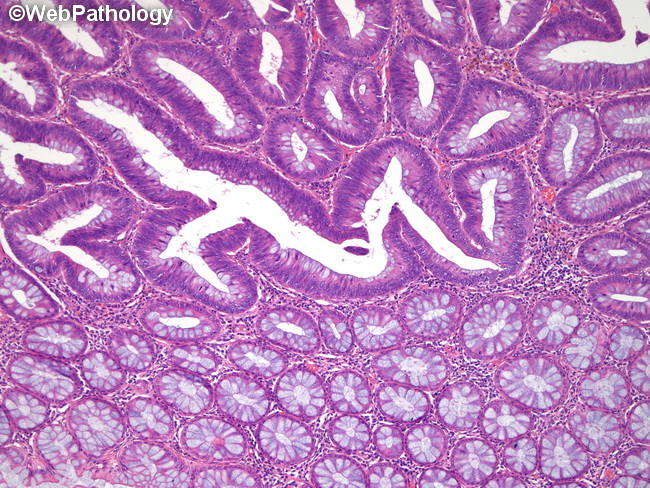
When associated with this syndrome, fundic gland polyps are removed because they can become cancerous. This rare, inherited syndrome causes certain cells on the stomach's inner lining to form a type of polyp called fundic gland polyp. For that reason, they are generally removed. Hyperplastic polyps are unlikely to become cancerous, although those larger than about 2/5 inch (1 centimeter) carry a greater risk.Īdenomas are the least common type of stomach polyp but the type most likely to become cancerous. Also known as gastritis, this condition can cause the formation of hyperplastic polyps and adenomas. The most common causes of stomach polyps are: Stomach polyps form in response to damage to your stomach lining. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
